Shoulder dislocation treatment in Burr Ridge
Also serving Plainfield, Morris and surrounding areas
Dislocated Shoulder Surgery Details
| Procedure | • Arthroscopic, Outpatient • Torn capsule and Labrum (Bankart lesion or Perthes lesion) are surgically repaired to restore stability to the shoulder joint. |
| Duration | 1.5 hours–2 hours |
| Anesthesia | General |
| Recovery | • Sling for 4-6 weeks. • Therapy begins at week 4 to allow time for early healing • Physical Therapy will last for 3–4 months • Return to work is dependent on type of work • Return to full sports is 4–5 months post-surgery. |
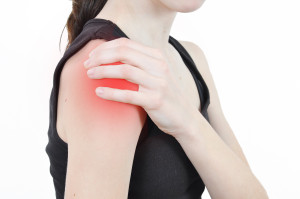
Causes of Shoulder Dislocation
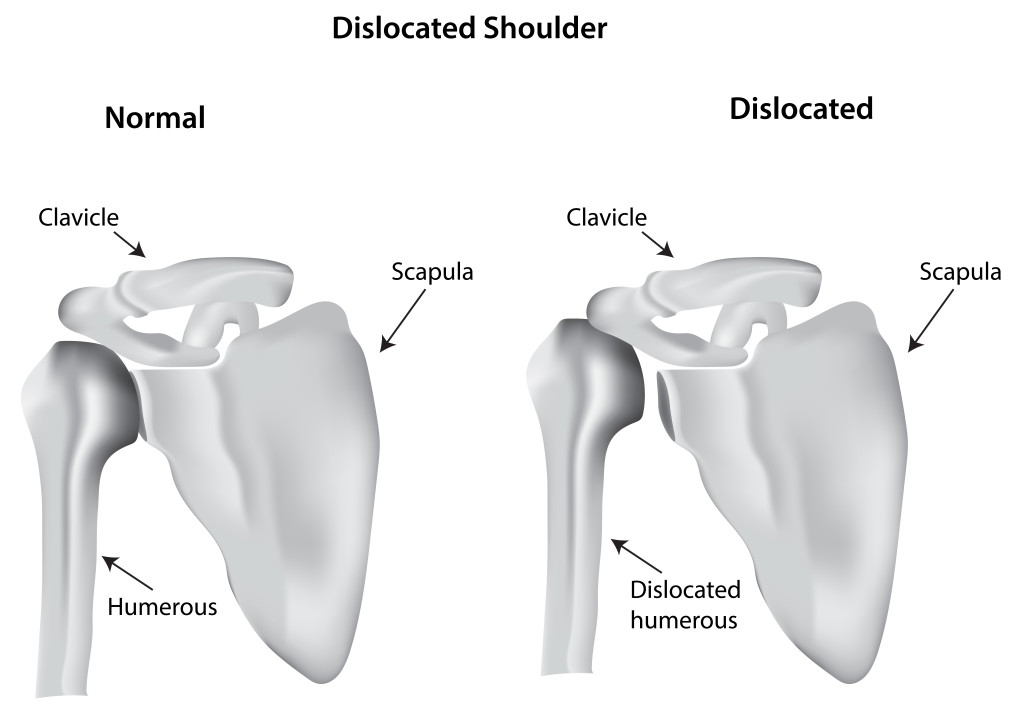
The shoulder joint consists of a ball and socket, and when these two become separated a dislocation occurs. There are many causes, but most commonly, some traumatic injury causes the dislocation such as sports injuries, work injuries, falls, or motor vehicle trauma. The shoulder may partially dislocate and return spontaneously to its normal position, or it may come completely out of socket and require medical attention to place the ball back in the socket. The most common form of dislocation is when the ball dislocates out the front of the socket.
Shoulder Dislocation through Age Groups
Younger patients (ages 25 and under) who are active in sports have a very high likelihood of repeat dislocation after sustaining their first injury. The chances range from 50%–90% that the shoulder will dislocate again. In this age group, a more aggressive treatment approach involving early Arthroscopic Surgical Repair of damaged ligaments and cartilage is becoming an acceptable norm, in much the same way a torn ACL is surgically treated early to stabilize the knee joint. Many studies now show significant benefit to early surgical repair of the dislocating shoulder joint in young athletes. There is a reduced chance of arthritis developing in the shoulder when earlier surgical intervention is undertaken for a dislocated shoulder.
Physical therapy will be enough to prevent repeat dislocation for many, but not all, patients in this age group, and treatment is individualized depending on activity level, type of sport, and desire for return to sports.
Older patients (ages 25 and up), are not as likely to have repeat dislocations. Treatment is based on ability to function in life and work. For people who do not re-dislocate, using a maintenance exercise routine may be all that is needed. For people who have instability or looseness in the shoulder that affects daily life or work, Arthroscopic Surgical Repair may be required.
Symptoms
Some of the most common symptoms include:
- Weakness, or numbness in the arms, extending down to the hands and fingers
- Extremely limited range of motion or complete inability to move the arm
- A shoulder that appears out of place
- Swollen or bruised shoulder
- Discoloration
- Muscle spasms
If you suspect you have a dislocated shoulder, you should seek treatment right away.
Prevention
It’s not always possible to prevent a shoulder dislocation. This injury, like many sports injuries, arises unexpectedly, so it is important to know what to look for and how to react to improve your chances of a quick recovery. However, staying safe during all physical activity can help you lower your chances of experiencing a shoulder dislocation. Keep the following preventative measures in mind:
- Ensure you are wearing the appropriate protective gear for your sport
- Understand the distinction between pain from injury and muscle fatigue, and discontinue participation if you begin to experience shoulder pain
- Take the recommended rest days to allow full-body recovery
- Thoroughly stretch before and after sports or working out
- Warm up before jumping into your activity
- Cool down after physical activities
Shoulder Dislocation FAQs
What causes a shoulder to dislocate?
Most cases of shoulder dislocation occur following an injury, such as a fall or a traumatic blow to the arm. Athletes are especially prone to shoulder dislocation, particularly if they participate in contact sports.
What are the types of shoulder dislocation?
The most common type of dislocation is anterior (ball dislocates out the front of the socket). Much less common are posterior dislocations (ball goes out the back of the socket) but these can occur with high energy trauma such as motor vehicles accidents, or during seizures. Subluxation means that the ball moved partially out of the socket in any direction, but not all the way out. These can occur with trauma and with various throwing sports such as volleyball, baseball, softball, and football.
How is a dislocated shoulder diagnosed?
When the ball is stuck outside the joint the patient is acutely aware and in pain. This is an emergency which requires immediate treatment to put the ball back into the socket. Most often this is at the emergency room or occasionally in a doctor’s office, or on the field of play. These cases are usually obvious with a deformed-appearing shoulder and will be confirmed with X-ray. Some patients will experience the ball spontaneously going back into the socket before emergency treatment is rendered. These situations still require orthopedic evaluation with X-ray and MRI.
A subluxation can be more subtle. Often athletes will feel a quick out and back in movement to the ball and socket of the shoulder. These injuries require evaluation by an orthopedic surgeon, along with X-rays and often MRI.
Is surgery necessary for shoulder dislocation?
Research and statistics show that younger age and athletic activity at the time of a first dislocation are high risk factors for repeat dislocation. For patients under age 25 and athletically active, the chance of repeat dislocations is 80%-90%. This chance of re-dislocation decreases with age and with lower athletic activity. For younger patients, surgery is often required. This will stabilize the joint, significantly reduce the chance for repeat dislocation, and help to prevent further damage and arthritis in the shoulder. Some patients may still do well with time and physical therapy alone, without surgery. Many athletes in season choose to rehab and attempt to return to play after the initial injury, and plan for surgical repair after the season.
How soon can an athlete return to sports after shoulder dislocation? If the shoulder is treated without surgery and rehabilitation is successful, athletes can return to play often within a month. When arthroscopic surgery is performed to repair a dislocated shoulder, it can take 6-8 months to return to sports. Return to play is guided by the surgeon and the physical therapy team throughout the rehabilitation process.
What are the risk factors for shoulder dislocation?
It is also important to be are aware of the risk factors associated with shoulder dislocation. Although anyone can experience a dislocated shoulder, certain things can put one at a higher risk:
- Participation in contact sports
- Age (people between the ages of 15 and 30 are more at risk)
- Prior shoulder dislocation
What complications are associated with shoulder dislocation?
Complications of shoulder dislocation are related to bone and tissue damage near the shoulder, such as:
- Fractures to the bone
- Sprains in the ligament and tendon
- Nerve damage near the injured area
- Blood vessel damage
- Muscle strain
Occasionally, individuals who dislocate their shoulder develop a type of injury known as a Hills-Sachs defect. It is akin to a dent in the bone and the injury impacts the humerus, which is the bone located in the upper arm. This injury has many of the same symptoms as shoulder dislocation, making it hard for patients to distinguish it from the original injury. However, Dr. Burt can diagnose the Hills-Sachs defect as he examines the dislocated shoulder with X-rays, MRIs, or CT scans.
Is it safe to pop my shoulder back in place while I wait for treatment?
In the event your shoulder becomes dislocated, do not attempt to push your shoulder back into place. Also, do not allow anyone who is not a specifically trained professional to move your arm, as doing so could lead to even more extensive damage.
Will I need other treatments after my shoulder is treated?
After your joint is treated, you may need additional treatment as part of your care plan. This may include:
Immobilization: Your arm may need to be placed in a splint or a sling to keep the shoulder in place. Immobilization is helpful in reducing the stress on the shoulder to promote healing. You may need to apply ice to the injured area throughout the day to help with swelling.
Medication: Medication may be prescribed to help you manage the pain and inflammation associated with shoulder dislocation.
Physical therapy: Physical therapy allows the patient to regain strength and range of motion in the shoulder. Physical therapy may include special stretches and exercises and can last for months after the shoulder dislocation.
Schedule an Appointment Today
Dr. David Burt is a renowned sports medicine physician who is dedicated to helping his patients live life free from chronic pain or discomfort. He specializes in treatment of shoulder injuries, and offers a number of treatment solutions to patients who suffer from shoulder dislocation. In addition to treating shoulder dislocations caused by sports injuries, Dr. Burt works with patients in need of a workers compensation surgeon. To learn more, or to schedule a consultation, contact his practice today at 815-267-8825. Dr. Burt proudly serves patients throughout Naperville, Joliet and Aurora, IL.
Recent posts
Lateral Decubitus Position for Arthroscopic Suprapectoral Biceps Tenodesis

The purpose of this report is to describe arthroscopic suprapectoral biceps tenodesis in the lateral decubitus position. Many technique descriptions for this procedure emphasize the beach-chair position to obtain optimal anterior subdeltoid visualization of the relevant anatomy. This is not...
Read MorePhysician's corner: Dr. David Burt

Two years ago, Dr. David Burt opened up his third clinic with Midwest Sports Medicine Institute in Burr Ridge. Along with locations in Plainfield and Morris, Dr. Burt is able to treat countless of athletes of all ages and levels...
Read More
