Meniscus tear surgery in Burr Ridge
Also serving Plainfield, Morris and surrounding areas
| Procedure | Arthroscopic, Outpatient |
| Duration | 45 minutes to 1 hour |
| Anesthesia | General |
| Recovery | 4–8 weeks of physical therapy. |
| Bracing | The majority will not need brace and this is only used when the meniscus has been sutured. |
The meniscus is a rubbery, shock-absorbing cartilage in the knee joint. Meniscus tears are commonly associated with sports injuries but can also occur without injury, during everyday activities. Meniscus tear symptoms include pain, swelling, locking, or catching in the knee. The symptoms may also fluctuate, with improvement for periods of time and spontaneous worsening at other times. Physical examination and MRI are used to define the injury and the recommended treatment is Arthroscopic trimming or repair of the torn meniscus depending on the type of tear. This is outpatient surgery and generally allows for immediate full weight bearing and no use of crutches or braces. Patients typically attend physical therapy for 3–4 weeks but may return to their daily activities as pain subsides.
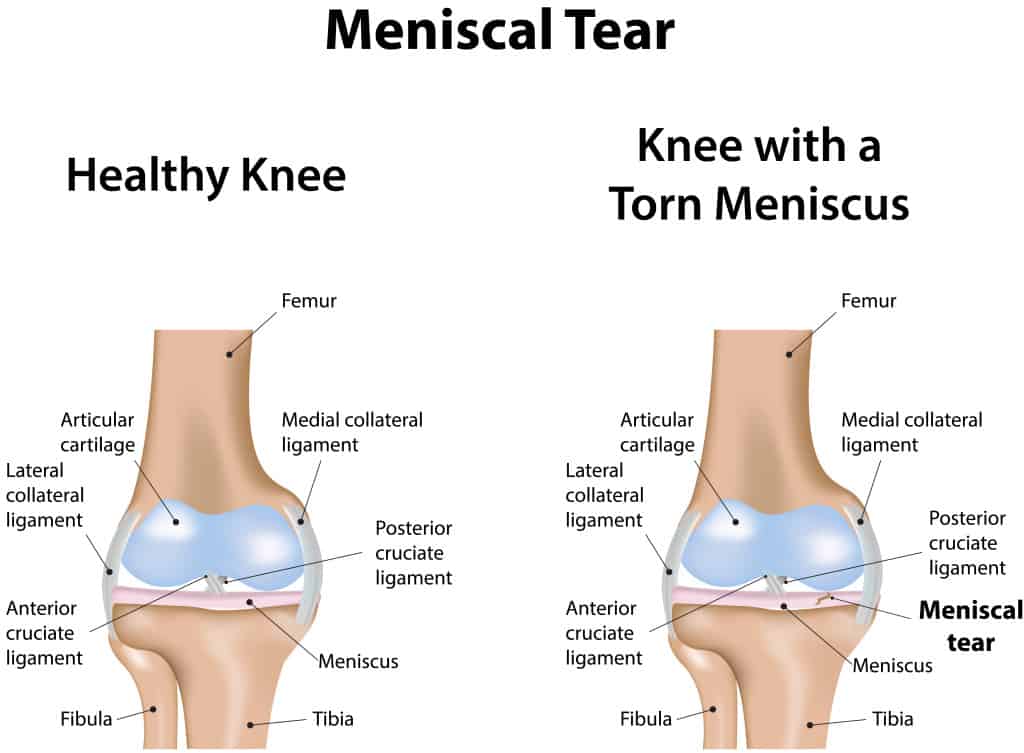
The majority of meniscus tear are in the avascular zone (no blood supply) of the meniscus and therefore do not heal on their own. They will continue to worsen and cause damage to other cartilage structures in the knee. Therefore, it is typically advised to remove the torn portion with arthroscopic surgery. In a smaller number of cases the meniscus tears near the periphery where there is good blood supply. In some of these cases placing sutures to repair the meniscus is advisable. These occur more often in traumatic injuries in younger athletes, such as with an ACL tear.
Meniscus Tear Recovery Time
The recovery after a meniscus repair is very different than recovery from trimming of the meniscus. It requires bracing, crutches, and 4-6 months of recovery time before returning to sports activities. Meniscus repair is performed in only about 5-10% of patients and is typically associated with a traumatic injury such as an ACL tear.
Meniscus Tear FAQs
Will surgery be necessary?
The degree of severity with a torn meniscus varies widely; and, as a result, treatment ranges from a conservative monitoring approach to physical therapy and surgery. Generally, meniscus tears do not heal on their own and ultimately may lead to substantial pain and instability. If there are no symptoms of any kind it may be appropriate to monitor or try physical therapy. If the tear is symptomatic it typically will require arthroscopic surgery. If the meniscus tear is in an area that has a blood supply, it may be repairable at the time of surgery. Tears closer to the center of the meniscus typically have to be trimmed at the time of arthroscopic surgery, as they have no capacity for healing.
Experienced Burr Ridge orthopedic surgeon Dr. David Burt knows that it is also important to consider the lifestyle, age and preferences of each patient when weighing treatment options. Whether you are a high-level athlete or an active individual, Dr. Burt is skilled in offering effective solutions for every type of injury, and every patient.
Is the meniscus removed during surgery?
The vast majority of meniscus tears are in the Avascular (without blood supply) part of the meniscus and the treatment in these cases is to remove the torn portion of the meniscus during arthroscopy. There are some tears less commonly that are in the Vascular (with blood supply) zone of the meniscus and these are repaired with sutures at the time of surgery. These are also commonly seen in patients with a newly torn ACL ligament. In either case the arthroscopic surgery is performed as outpatient surgery with minimally invasive techniques, and patients begin physical therapy immediately after surgery as a part of their recovery.
How can I prevent meniscus tears?
One of the most important strategies for prevention is to maintain good strength and flexibility from “core to floor,” which means low back, core, hip, and legs. When you strengthen muscles in your legs, hips and abdomen, you are taking pressure off the knee. If the meniscus is supported by your muscles, it will be subjected to less direct force. In this case the chances of suffering a tear are greatly reduced.
Another way to minimize your chances of suffering a meniscus tear is to choose physical activities that match the condition of your knee, as well as your overall fitness. If you are playing high-impact sports, make sure your muscles are ready for it. Even when your fitness level is superb, it is prudent to avoid situations in which your knee may become twisted.
Parents should be aware that children whose muscles are still developing are at risk of developing a meniscus tear when playing sports for the first time. This is especially true with football, basketball and soccer.
Older patients are also at higher risk for developing meniscus tears. It is important to modify exercises to stay lower impact and to avoid deep flexion of the knee such as with lunges and squats. Going past a 90-degree bend in the knee with any of your workout activities can put you at risk for a meniscus tear. A torn meniscus, together with the attenuated cartilage that is a normal part of aging, may lead to knee arthritis. Without the cushioning effect of the meniscus and supportive cartilage, bones will come in contact during movement of the knee, generating significant pain. In addition, if part of a torn meniscus migrates into the joint, the knee may feel as if it is slipping, popping or locking, and it may be very painful.
Why is my meniscus important?
The meniscus is crucial for knee joint function. It consists of two C-shaped pieces of fibrocartilage positioned between the thigh bone (femur) and the shin bone (tibia). These structures serve several vital roles:
- Shock Absorption: They help distribute weight and absorb shock during activities such as walking, running, or jumping.
- Stability: By deepening the tibial plateau where the femur meets the tibia, the meniscus enhances joint stability.
- Lubrication: The meniscus aids in lubricating the joint, reducing friction during movement.
- Load Transmission: More than half (50 to 70%) of the load transmitted through the knee passes through the meniscus, highlighting its role in joint preservation.
What are the signs and symptoms that I’ve torn my meniscus?
A torn meniscus typically presents with several indicative symptoms:
- Pain located on the side or center of the knee, often worsening with twisting or squatting movements.
- Swelling usually develops within 24 to 48 hours due to inflammation.
- A popping sensation when the tear occurs.
- Limited motion, such as difficulty fully straightening your knee, often described as feeling “locked” or “stuck.”
- A sensation of instability with your knee feeling like it may give way under stress.
Are meniscus tears preventable?
While not all meniscus tears can be prevented — due to factors like age-related degeneration or genetic predisposition — certain measures can reduce the risk:
- Strength Training: Strengthening the muscles around the knee, particularly the quadriceps and hamstrings, can help stabilize and protect the joint.
- Flexibility: Regular stretching to maintain knee and leg flexibility can prevent undue stress on the menisci.
- Proper Techniques: Using correct form during sports and activities can minimize harmful twisting forces on the knees.
- Avoid Overloading: Managing load during activities, especially in sports that involve heavy lifting or sudden changes in direction, can help protect the knee.
What are the long-term success rates for surgery on the meniscus?
The success rates for meniscal surgery, particularly meniscectomy (removal of damaged meniscal tissue) and meniscal repair, vary depending on factors like the type of tear, patient age, and overall knee health, which makes personalized consultation with Dr. Burt and treatment planning essential. Generally:
- Meniscectomy: Has good short-term results in relieving pain and improving function but may lead to higher rates of osteoarthritis in the long term.
- Meniscal Repair: Shows better long-term outcomes in terms of preserving knee joint health and preventing arthritis, particularly in younger patients with specific tear types (like longitudinal tears in the vascular outer zone). Studies indicate success rates of 85% or higher for preserving knee function.
Can the meniscus tear a second time?
Yes, the meniscus can tear again after either a surgical repair or natural healing. Re-tear rates vary:
- After Meniscal Repair: Re-tears are more common in the first few months post-surgery while the tissue is still healing. The risk can be influenced by the initial tear’s location and type, as well as postoperative rehabilitation and return to activity.
After Meniscectomy: Subsequent tears or degenerative changes can occur, especially if a significant amount of meniscal tissue was removed.
Learn More About Meniscus Tear Recovery in Chicago
As leading Chicago area orthopaedic surgeons, Dr. David Burt treats a number of knee injuries, including meniscus tears. At their state-of-the-art practices in Burr Ridge, Plainfield, and Morris, Dr. Burt thoroughly diagnoses each patient to determine the extent of injury before making a treatment recommendation, typically physical therapy or outpatient surgery. Learn more about meniscus tears by contacting Midwest Sports Medicine Institute to schedule a consultation.
Recent posts
Lateral Decubitus Position for Arthroscopic Suprapectoral Biceps Tenodesis

The purpose of this report is to describe arthroscopic suprapectoral biceps tenodesis in the lateral decubitus position. Many technique descriptions for this procedure emphasize the beach-chair position to obtain optimal anterior subdeltoid visualization of the relevant anatomy. This is not...
Read MorePhysician's corner: Dr. David Burt

Two years ago, Dr. David Burt opened up his third clinic with Midwest Sports Medicine Institute in Burr Ridge. Along with locations in Plainfield and Morris, Dr. Burt is able to treat countless of athletes of all ages and levels...
Read More
